Definition of Migraine

Pathophysiology
The pathophysiology of migraine is not completely understood. The neurovascular theory posits that migraine pain originates from the trigeminovascular system, the activation of which triggers the release of vasoactive neuropeptides, which in turn triggers vasodilation and dural plasma extravasation, leading to neurogenic inflammation.
Another way to say this is that the trigeminovascular system can go awry and cause inflammation as well the enlargement of blood vessels in the brain, thereby leading to pain in the head.
Prevalence and Burden of Disease
Episodic Migraine
Four Phases of a Migraine
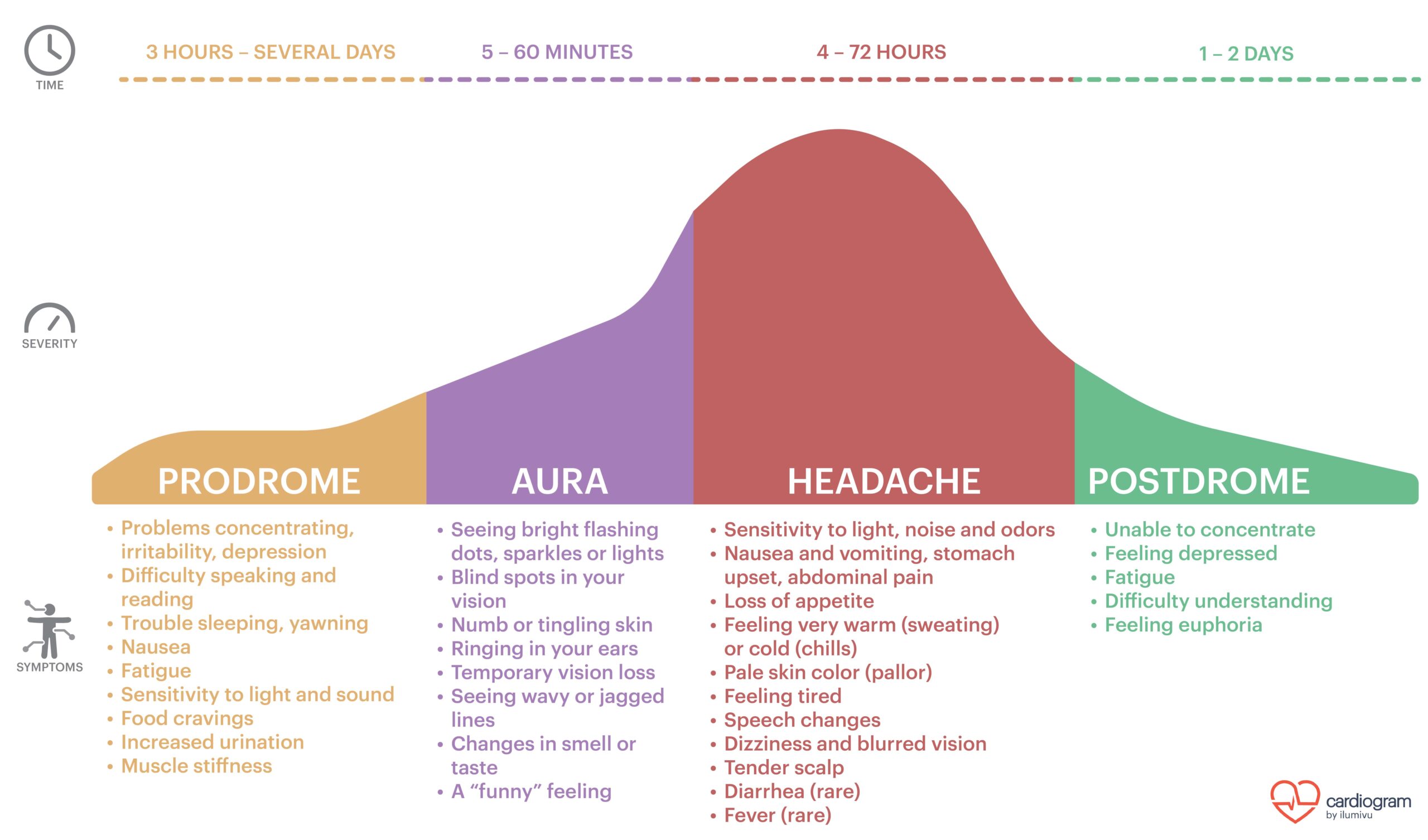
Most (and possibly all) migraine episodes are preceded by a prodrome that lasts for a few to many hours. Common prodromal symptoms include irritability, food cravings, sensitivity to light or sound, or difficulty concentrating. Approximately 20% of migraineurs experience an aura for 5-60 minutes, during which time they may experience visual disturbances, temporary loss of sight, or numbness and tingling in parts of the body. The headache phase follows either the prodrome or the aura. This phase typically lasts 4-72 hours. Headache is often the predominant symptom, but associated symptoms such as nausea, vomiting, anxiety, sensitivity to light, smell, and/or sound, or neck pain/stiffness are almost always present and can be temporarily debilitating in and of themselves. After the headache phase has run its course, the postdrome phase sets in. This phase typically lasts 24-48 hours and can manifest in a variety of ways, including fatigue, depressed mood, or euphoric mood.
Prevention
Treatment
Early Detection: The Holy Grail of Migraine Treatment
The Holy Grail of migraine treatment (as opposed to prevention) lies in the earliest possible detection of a developing migraine episode, well before the onset of headache. Little research has been published to-date on this topic. However, one study used sleep time data from the wrist-worn Empatica E4 wearable sensors, but their findings were inconclusive (2). A systematic review of computerized migraine diagnostic tools identified 41 eligible studies, all of which focused on migraine diagnosis but not early detection (3).
Cardiogram's Early Migraine Detection Project
This is where we come in. We believe that with the right algorithm, a wearable has the potential to detect the subtle signals and alert a migraine sufferer to the oncoming migraine, even before a they themselves would likely be able to. And we believe that with enough data and input from our members, our data scientists can build that algorithm, which would then become a permanent feature in Cardiogram.
We've launched a migraine project and are asking our Cardiogram members who suffer migraines who are willing to participate to take our survey, and log their migraines in the app. Interested in contributing? Learn how here.
(1) https://www.alliedmarketresearch.com/migraine-drugs-market
(2) Siirtola P, Koskimäki H, Mönttinen H, Röning J. Using Sleep Time Data from Wearable Sensors for Early Detection of Migraine Attacks. Sensors (Basel). 2018 Apr 28;18(5):1374. doi: 10.3390/s18051374. PMID: 29710791; PMCID: PMC5981434.
(3) Woldeamanuel YW, Cowan RP. Computerized migraine diagnostic tools: a systematic review. Ther Adv Chronic Dis. 2022 Jan 24;13:20406223211065235. doi: 10.1177/20406223211065235. PMID: 35096362; PMCID: PMC8793115.



