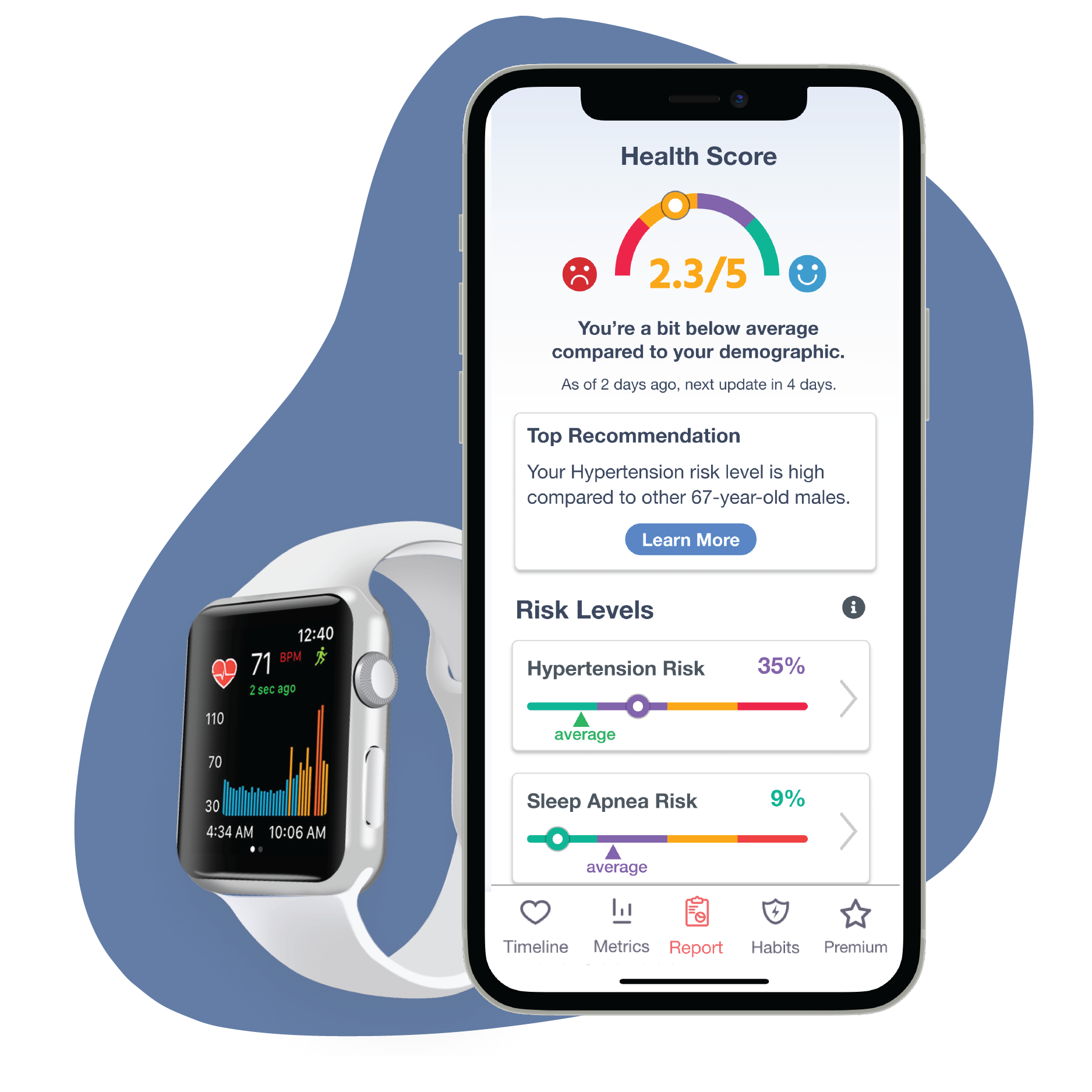
Rewind from where we left off in Part 1… I was at work, doing my typical duties (assessing and treating patients, completing diagnostic testing, etc.) when I started receiving alerts from my fitness watch that my heart rate was 180bpm. I also had mild chest pain, a little shortness of breath, and felt lightheaded.
I waved it off thinking it would resolve itself, though I kept my eyes on it. When, after some time, it persisted, I decided to inform the doctors. They asked many questions about my symptoms as they witnessed my high heart rate and very low blood pressure and asked if I needed an ambulance. I decided to drive myself to the hospital.
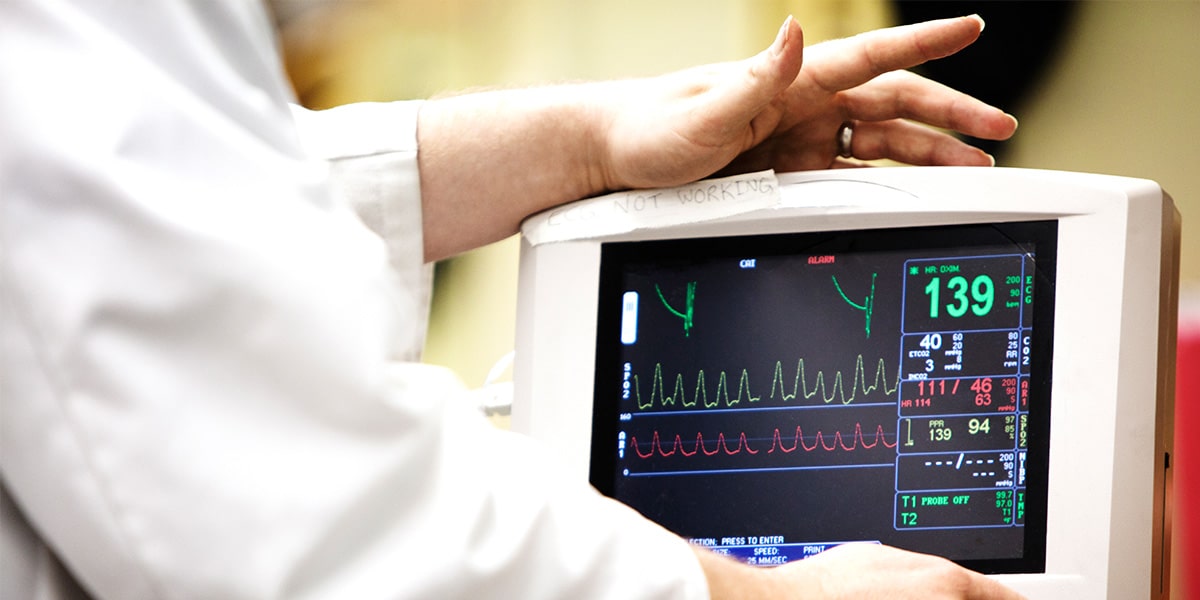
While at the ER before any imaging or lab testing, my heart rate settled back to normal. But (knowing something was off) I used my better judgment and decided to stay long enough for testing to be ordered and completed.
Sure enough, not long after I got back home from all testing, I was called and advised to return to the hospital due to severely abnormal lab values. I was told that I was on the brink of a heart attack due to elevated troponin (a cardiac lab indicator of a heart attack). Thankfully, though abnormal, the troponin levels were not high enough to register as a heart attack. I was admitted for several days to be monitored with a cardiac Holter monitor, diagnosed with Supraventricular Tachycardia (SVT), and put on beta blockers.
Another high lab value was creatine kinase (CK) which aligns with troponin and signifies heart damage or problems. My electrolytes (potassium, calcium, sodium, magnesium, etc.) were significantly low so I was also dehydrated. Low electrolyte values can also cause heart palpitations, causing my heart rate to jump to 160bpm-180bpm. After 20-30 minutes at this rate, I was in cardio exercise mode. Now image 6 whole hours of this. Not to mention, anytime an adult heart is racing like this, it’s under stress which can cause heart damage.
I had difficulty making a cardiology appointment and was back and forth to the ER with a racing heart and other accompanying symptoms. One time, I randomly showed up at the cardiology office that my discharge papers referred, hoping to be seen. I told the front desk my symptoms and was told I could wait around to see if any patients were no-shows so I could be seen. I waited for hours. The cardiologist agreed to see me and gave me a full workup, captured heart images with an echocardiogram, and completed a treadmill stress test (my very first experience). My stress test was great and I was told that my heart was okay. I explained my exercise regimen as the reason and that something needed to be done about my random high heart rate. Nothing.
I had been turned away by doctors at least 5 times in a matter of weeks complaining of random high rates, low blood pressures, chest pain, headaches, and mini seizures. And during that time, physicians constantly tried convincing me that my heart rate was fine.

I couldn’t capture the heart rate events
A lot of my really high heart rate events occurred in my sleep. During one visit, I was prescribed a beta blocker to take, as needed, and potassium supplements. Being that my resting rate is typically 40bpm, after 2 doses of the lowest dose of the beta blocker, my resting rate dropped to 25bpm.
I returned to cardiology again, and this time he brought in an electrophysiologist (a cardiologist that studies, specializes, and treats issues with the electricity of the heart.) With both doctors present, I explained everything, and they told that I may need an ablation or an implanted pacemaker device. I did not understand why. Then, they brought in ‘pacemaker’ talk after one visit, again disregarding my workout regimen. So, to simply describe this, if I had a high rate, I may need ablation; if my rate was too low, then I may need a pacemaker. I did not want a pacemaker or ablation; I was 29 years old!
I followed up with electrophysiology and wore a Holter monitor, but only for 24 hours. (Not long enough to get sufficient data for the correct interventions.) My issues with my heart rate continued and I went through a series of tests: from additional stress testing, electrocardiograms, bubble studies, a specialized echocardiogram used to detect a hole in the heart, additional lab testing, (at one point I was told my high heart rate may be caused by the functioning of my thyroid gland), diagnosed with costochondritis, (inflammation of the chest cavity) also because I was constantly nauseous, I was also checked for autoimmune diseases such as Sickle Cell and Lupus, and had more seizure episodes. None of the tests came back with the clarity needed, so cardiology, neurology, and primary all brushed my symptoms to the side.
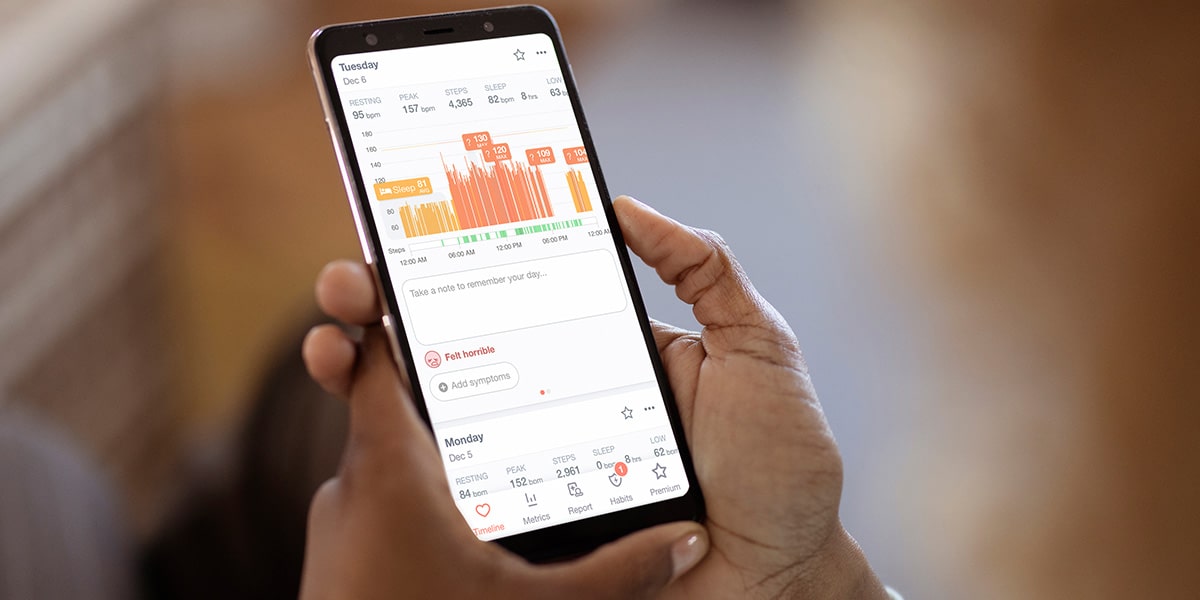
I took time off from work to research heart issues, symptoms, and tests myself so I could ask the right questions. I was already routinely wearing my fitness watch to bed to monitor my heart, but the intermittent heart rate checks were not enough to satisfy doctors.
Somewhere along the way, I found Cardiogram; it was a turning point in my journey. One of the main things that attracted me was the design of the app and its continuous heart rate recording feature that mimicked continuous heart rate monitoring of doctor-ordered Holter monitors. Cardiogram also featured teachings of various cardiac related parameters such as resting heart rates and peak/low heart rates. With Cardiogram, I was finally able to capture a 232bpm and other 140-180bpm events. Not only was I able to capture those rates and show them to doctors, but I was able to show them how long I stayed in those rate ranges.
I was soon back in the ER after experiencing severe muscle aches, delirium, presyncope, nausea, chest pain, etc. No elevated troponin, but my CK levels were in the thousands. I was given fluids for dehydration and instructed to rest and only partake in ‘activities as tolerated’.
I felt okay and soon returned to work. Less than 48 hours later, I returned to the same ER with worsened symptoms and honestly didn’t even remember driving myself to the ER. My CK levels had tripled and at this point, I was diagnosed with rhabdomyolysis, a muscle breakdown that can damage the kidneys. Rhabdomyolysis is seen after extensive, intense exercising, or drug use, following critical dehydration levels. Rhabdomyolysis can be fatal.
With my heart still working overtime, I followed up with electrophysiology and with my Cardiogram data, I finally got the physician to better understand my condition. I showed them my timestamped high/low rates, durations, alongside my exercise activities and timestamped check-ins at my local gym through. Cardiogram helped me to finally prove that I was not working out during those late night very high rates. Because of this, an additional 6 weeks of Holter monitoring was ordered that ended up backing my Cardiogram claims. Next, I was finally scheduled for cardiac ablation.
Stay tuned for Part 3/3...
Shaquana, also known as Shay, is a cardiovascular technologist who is also passionate about fitness and wellness. She generally loves helping people (including helping them reach fitness goals). Shaquana also enjoys healthcare research, exercise physiology, and sports at large.