We’ll start here. Because really, what is cardiac ablation? Well, it’s when electrophysiologist (remember, an electrophysiologist is a cardiologist that specializes in the treatment of the electricity of the heart) go into the heart with a cardiac catheter (thin flexible tube) and repair or destroy parts of the heart tissues responsible for the arrythmias.
The cardiac catheter itself is generally inserted through the groin but, per case, it may be inserted through the neck. Cardiac ablation is usually coupled with an electrophysiology study ahead of the ablation. And an electrophysiology study is simply the cardiologist studying measuring the possible reasons of the arrhythmia.
Each ablation is different, and they are ordered and performed for different reasons. And, as all bodies respond differently, each requires different pre and post instructions.
Now, for my part of the story:

Anything pertaining to studying or repairing tissues of a major organ can be scary. Initially, I was okay with the news that I would need an ablation as my doctors assured me that everything would be okay and explained the process. I also watched videos on cardiac ablation for better understanding.
For me, the most comforting part of the doctor’s explanation was that cardiac ablation is a procedure and not surgery; it does not require opening the chest. It also helped to know that cardiac ablation has a high success rate and, without complications, only takes about an hour to complete. The procedure also includes mild to moderate sedation. Of course, each case is different as some individuals experience complications and/or have more than one cardiac ablation.
The prepping was simple with activities as tolerated (what had already become the story of my SVT diagnosed life); sets of laboratory test completed days before, NPO – nothing by mouth (or fasting) after midnight, dressing comfortably, and arriving by 0600 with preparations to stay for 24 hours. I have met ablated individuals who went home an hour after the procedure, though some longer.
I started to feel frightened the morning of the ablation. Naturally, I was worried about things going wrong. I was wheeled away, hoping to rid the SVT. I remember laying on the exam table in the cardiac catheterization lab (cath lab, for short) under lots of lights and nurses and staff all around me prepping for the procedure. I was draped and informed on the medications I was to be given via I.V., with one being a medication to help me relax.

I was wheeled to observations. I was bandaged in my groin area - the catheter insertion sight. I stayed overnight to be monitored, was given a prescription for pain medicine, and was told I may still experience irregular heartbeats for up to a few weeks after the ablation. I was advised to take more time off from work; I took 1 week sick time. Again, I was told activities as tolerated, no caffeine, and no high intensity workouts. Basically, I needed to rest and to follow up with the electrophysiologist in 1 week.
I still had bouts of rapid rates – yes, still in the middle of the night – and I continued to monitor my rates with Cardiogram compare them to ratings from various devices; randomly comparing rates of a chest strap monitor, gym equipment, my fitness watch, and Cardiogram, everything aligned. Prior to the ablation, I had normal worries of going to bed and never waking up, which did continue. And when I followed up with electrophysiology, I was put on a 1-week Holter monitor. In truth, I think this was ordered to appease me and ease my worries.
Say it with me, “Break Through.” Everything changed. The doctors were listening. I was in a better space, though still afraid of returning to my regular activities. Those who work out regularly can relate to the indescribable feelings when unable to work out.
Once again, I will say that each ablation case is different. Personally, I went through bouts of unrelated symptoms that causes some palpitations and was ordered another Holter monitor for 4 weeks. Electrophysiology questioned me when no ‘target heart rates’ were captured on the Holter report. This was because I was still afraid to run. An additional 2 weeks of wearing the Holter was ordered, and I was advised to run and do other cardio exercises while wearing it. The additional data revealed some really high rates, but we discovered these to be during my workouts when my gym log’s check-in times matched the timeframes of those high rates.
I often share my SVT and cardiac ablation advocation and medical gaslighting experience with anyone who shares similar obstacles; simply hearing that I had a good experience with cardiac ablation often eases some of the stress and worries. It brings an indescribable level of comfort when being assessed by someone that experienced a similar cardiac journey.
With my own experience, I now often bridge the gaps between patients and doctors as sometimes it is difficult for patients to verbalize symptoms and thoughts to someone who have not experienced similar obstacles.
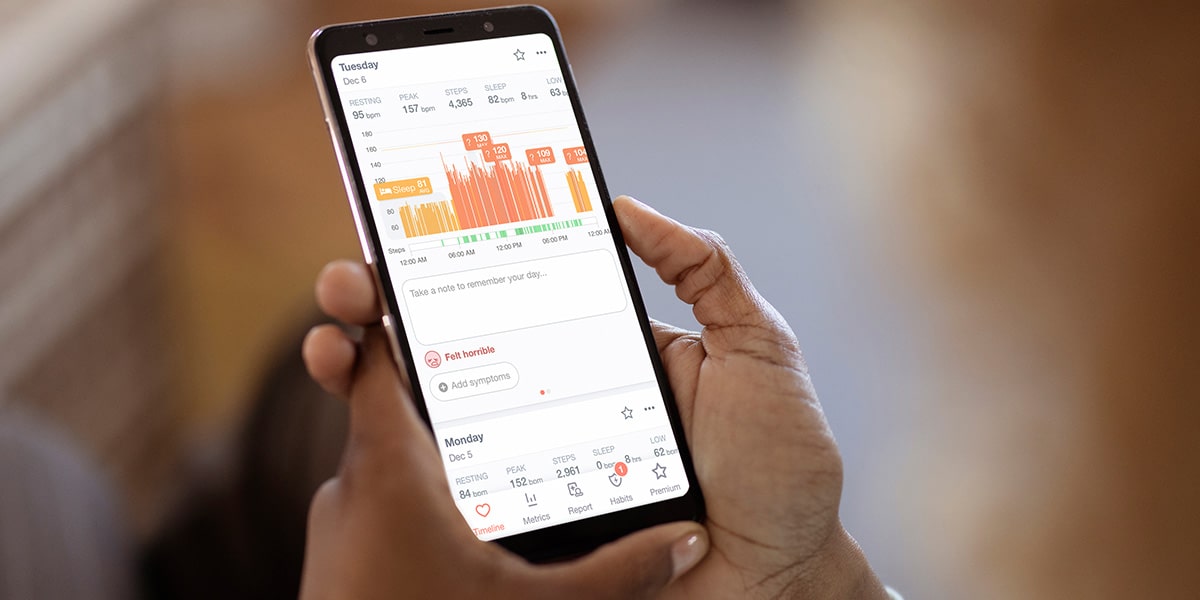
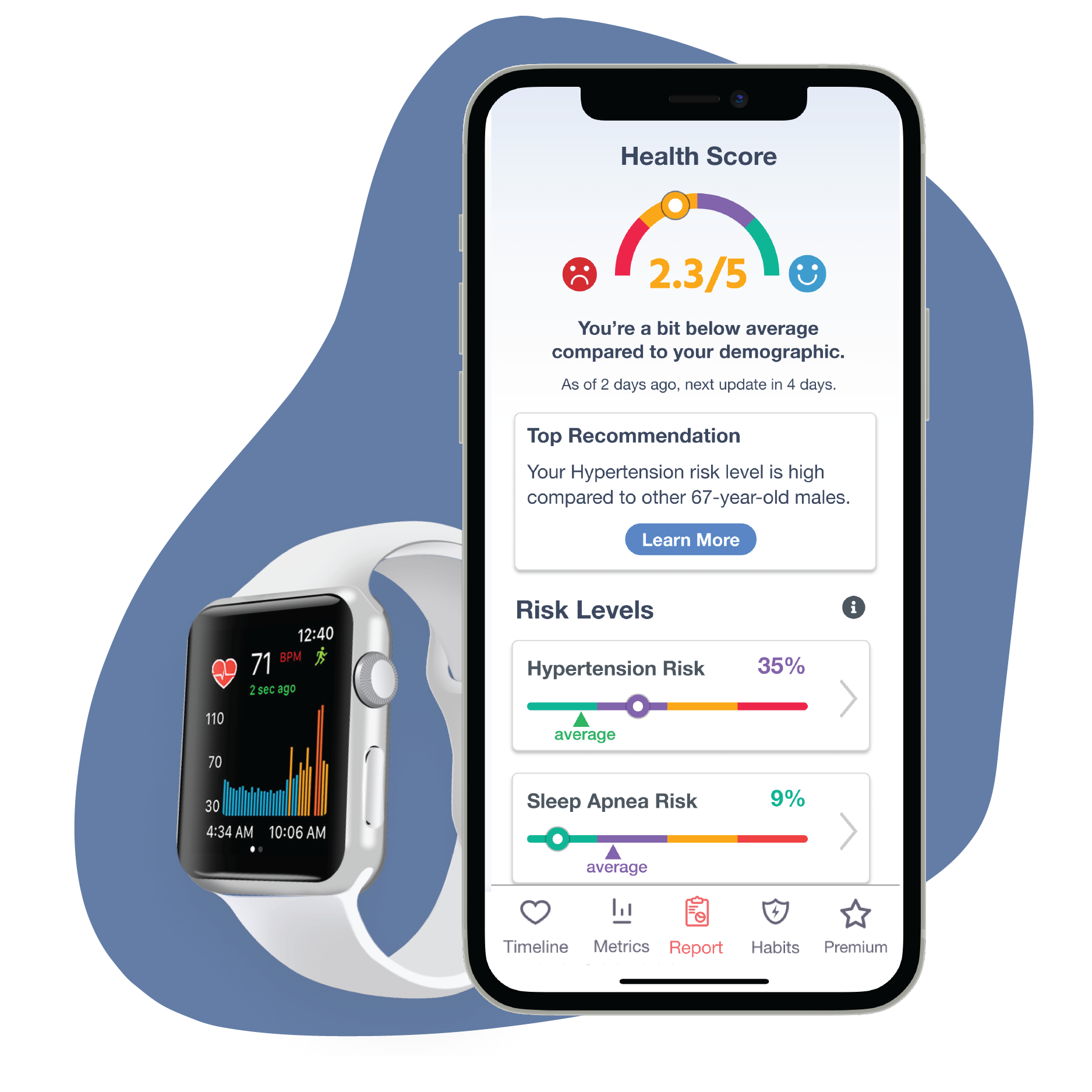
With each cardiac topic, I share and recommend Cardiogram and its teaching features to everyone that sparks an interest; especially to those who already have fitness trackers.
Cardiogram helped me get doctors to finally understand my symptoms. Cardiogram is a huge part of my cardiac health, fitness, and overall wellness. To this day, I consistently review my Cardiogram app with each workout since becoming a member 6 years ago.
Shaquana, also known as Shay, is a cardiovascular technologist who is also passionate about fitness and wellness. She generally loves helping people (including helping them reach fitness goals). Shaquana also enjoys healthcare research, exercise physiology, and sports at large.